Diagnostics
Arterial Brachial Index (ABI)
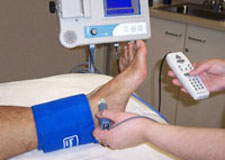
People with PAD are at increased risk for heart disease and strokes. PAD can also be an indicator of diabetes, hypertension and other conditions.
The ABI test is simple. It uses uses a standard blood pressure cuff and a special ultrasound stethoscope called a Doppler. The pressure in the ankle is compared to the pressure in your arm to determine how well the blood is flowing and whether additional testing is needed.
Early detection of peripheral arterial disease can help prevent amputation, heart attack and stroke.
Peripheral Arterial Disease of the arteries that affects 10 million Americans. It can affect anyone regardless of age but is most common in men and women over the age of 50. Over the age of 65 it affects as much as 20 percent of the population.
24-Hour Holter Monitoring
A Holter monitor is a portable EKG that monitors the electrical activity of a freely moving person’s heart, generally for one to two days, 24 hours a day. It is most often used when the doctor suspects an abnormal heart rhythm or ischemia, which means not enough blood flowing to the heart muscle.
It is a painless test – electrodes from the monitor are taped to the skin. Once the monitor is in place, you can go home and perform all of your normal activities, except showering. You will be asked to keep a diary of your activities, any symptoms you experience and when they occur.
What is an event monitor?
If your symptoms are infrequent, your doctor may suggest an event monitor. This is a device that, when you push a button, will record and store the heart’s electrical activity for a few minutes. Each time you develop symptoms you should try to get a reading on the monitor. They are used for weeks to months, typically one month. This information can later be transmitted by telephone to the doctor for interpretation.
What is a Holter scan?
After the patient wears the Holter monitor for a 24-hour period, he or she brings the monitor back and a technician scans through more than a hundred thousand beats looking for any irregular rhythms or rates. The technician interprets the findings, creates a written report and has it reviewed by an electrophysiologist. Finally, the report is sent to the referring physician.
Event Recording/Monitoring
The Cardiac Event Monitor is small device, about the size of an iPod, that is worn on the chest and is used to detect abnormal heart rhythms. When patients feel an “event,” such as dizziness, weakness or palpitations, they push a button on the device. The monitor stores the event and it is later sent over a telephone line to the cardiologist for review.
This test allows for on-demand heart monitoring outside the office setting as patients go about their normal routine. The monitor can be worn for up to 30 days and is only removed for bathing.
Electrocardiogram (EKG)
An EKG shows how fast the heart is beating and shows its rhythm (steady or irregular) in 12 different places on the body at the same time. It also records the strength and timing of the electrical signals as they pass through each part of the heart.
An EKG can help reveal a number of heart problems. This is especially true if doctors can compare a current EKG recording to an older one. EKG recordings can also reveal. An EKG can help doctors diagnose:
• A Heart attack, whether it is happening now or has happened in the past.
• Lack of blood flow to the heart muscle
• An irregular heartbeat
• A heart that does not pump forcefully enough
• Disease in the heart valves between the different heart chambers
• Birth defects in the heart.
Echocardiogram
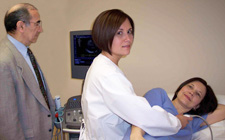
An Echocardiogram is an ultra-sound of the heart. It uses sound waves to create a moving picture of the heart that is more detailed than x-ray and involves no radiation exposure.
A trained sonographer performs the test, then your physician interprets the results. An instrument that transmits high-frequency sound waves called a transducer is placed on your chest near the breast bone and directed toward the heart. The transducer picks up the echoes of the sound waves and transmits them as electrical impulses, which are then converted into moving pictures of the heart. In the photo, Dr. Salimi observes the heart’s image on the monitor as the Medical Assistant scans the patient.
Stress Testing
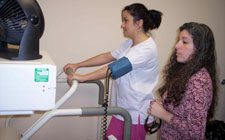
A stress test demonstrates the effect that exercise has on your heart. In a standard stress test, the patient walks on a treadmill while being monitored by an electrocardiogram (ECG) and blood pressure readings. This measures your heart’s reaction to your body’s increased need for oxygen.
The test continues until you reach a target heart rate, unless complications such as chest pain or an exaggerated rise in blood pressure develop. The heart is monitored for 10 to 15 minutes after exercising, or until it returns to its baseline heartbeat.
A stress test is performed to determine causes of chest pain, the exercise capacity of the heart, appropriate exercise levels in those beginning an exercise program, and to identify rhythm disturbances during exercise. There may be additional reasons that your health care provider requests this test. In the photo above, Dr. Donna Konlian attends a stress test in progress..
Nuclear Stress Testing
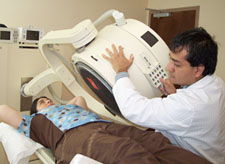
A nuclear stress test shows how well blood flows into the heart when it is at rest and during activity. A radioactive dye is injected into a vein and allows images to be taken that show how blood flows through the bloodstream and into the heart muscle. While the patient is reclined on a table, a camera is used to record images.
The scans are recorded when the heart rate is elevated and again when it is at rest. This allows the cardiologist to compare how well blood flows to the heart when the body is at rest, versus when it is active.
In comparison to the standard treadmill stress test, a nuclear stress test is more accurate and provides additional information. In the photo at left, Nuclear Medicine Technologist Freddie Chapal prepares for a test.
Stress Echocardiogram
The stress echocardiogram combines an echocardiogram with the standard treadmill stress test. It tests the heart’s reaction during periods of rest and exercise. The echocardiogram uses high-frequency sound waves (ultrasounds) to look at how the various parts of the heart work. If Coronary Artery Disease is present, the stress echo will often note changes in how the heart muscle contracts.
Pharmacologic Stress Test
A pharmacologic stress echocardiogram (echo) is a non-exercise test used to detect coronary artery disease (CAD), or a blockage of blood flow to the heart. The test provides a complete picture of the workings of the heart during periods of rest and exercise.
During the exam, a medicine is given to increase the rate and force of your heartbeat similar to exercise. Then the echo uses high-frequency sound waves (ultrasounds) to look at how the various parts of the heart work. If CAD is present, the stress echo will often note changes in the heart muscle contractions.
Pacemakers and Defibrillators Clinic
Advanced Cardiology Practice offers follow-up assistance for patients who have recently received a pacemaker or defibrillator. This includes periodic routine visits that can help detect problems and prevent symptoms from affecting your independence and activities of daily living.
When Do Follow-up Services Start?
Follow- services should begin within seven to 10 days after your pacemaker has been implanted. It is recommended that you bring someone to accompany you for this first appointment. This visit typically lasts about one hour, during which you will receive a monitoring unit, or “transmitter,” along with complete instructions for its use.
Transtelephonic Monitoring
About one month following implantation you will be scheduled for a telephone test. At an appointed time, our technician will call you at home to test your device over the phone. This test takes less than five minutes and the results are reviewed at its conclusion. Each test is reviewed by your cardiologist and recorded in your medical file.
Threshold Testing
Pacemaker clinic visits are referred to as “threshold testing.” These visits occur once or twice a year as prescribed by your physician. A registered nurse trained in pacemaker device therapy performs this evaluation, which takes approximately 30 minutes. The nurse checks your vital signs and discusses possible pacemaker-related symptoms. The nurse also examines your pacemaker pocket and performs a series of noninvasive, painless tests to analyze the pacemaker’s function.
The pacing system includes the pulse generator, the lead(s) connecting the pacemaker to the heart and you, the patient. Threshold testing helps the nurse determine if your pacemaker settings are programmed appropriately. Correct settings increase the longevity of the pacemaker generator. The test results are interpreted by a cardiologist and kept in your record.
Follow-up for Other Devices
Internal cardioverter defibrillator (ICD) follow-up is similar to pacemaker clinic visits. The appointments last approximately 45 minutes and can be as frequent as every three months.
A nurse will check your vital signs and perform an analysis of your ICD. Following this analysis, your results are reviewed by the cardiologist.