Your Heart & Vascular System
The following are some of the more common treatments that are routinely performed by our cardiologists, either in our offices or in the hospital.
Cardiac Catheterization/Coronary Angiogram
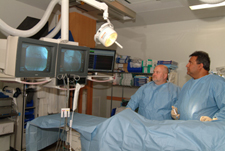
Your doctor uses cardiac catheterization to:
• evaluate or confirm the presence of heart disease (such as coronary artery disease, valve disease or disease of the aorta)
• evaluate heart muscle function
• determine the need for further treatment (angioplasty or bypass surgery)
The x-ray camera is used to take photographs of the arteries and heart chambers. When all the photos have been taken, the catheter is removed.
The cardiac catheterization procedure only takes about 30 minutes but requires several hours from the preparation through the recovery time.
Interventional Procedures
During the catheterization, if a blockage is identified, or if the cardiologist determines it is necessary, an interventional procedure may be performed to open narrowed coronary arteries to improve blood flow to the heart. Various interventional procedures are available, including:
Types of Angioplasties
A procedure in which a small balloon at the tip of the catheter is inserted near the blocked or narrowed area of the coronary artery. When the balloon is inflated, the fatty plaque or blockage is compressed against the artery walls and the diameter of the blood vessel is widened to increase blood flow to the heart. There are several types of Angioplasty:
Lower Extremity Angioplasty; Carotid Angioplasty; Renal Angioplasty;
In addition, patients who have had strokes, dizziness or fainting spells may have blockages in the carotid arteries (the arteries that supply the brain). In the past surgery was the only alternative. Now we can offer carotid angioplasty and stent placement without the need of general anesthesia and prolonged hospital days to open these arteries.
Similar angioplasty and stent techniques can be applied to the kidney arteries to treat patients with severe high blood pressure.
Laser Angioplasty
A laser device is utilized to open blocked arteries in the chest, legs and heart by pulverizing plaue that lines the arterial walls.
Angioplasty with Stenting
In most cases, balloon angioplasty is performed in combination with the “stenting” procedure. A stent is a small, metal mesh tube that acts as a scaffold to provide support inside the coronary artery. A balloon catheter is used to insert the stent into the narrowed artery. Once in place, the balloon is inflated and the stent expands to the size of the artery and holds it open. The balloon is deflated and removed, and the stent stays in place permanently. During a period of several weeks, the artery heals around the stent.
Angioplasty with stenting is most commonly recommended for patients who have a blockage in one or two coronary arteries. If there are blockages in more than two coronary arteries, coronary artery bypass graft surgery may be recommended.
Transesophageal Echocardiogram (TEE)
If a standard echocardiogram is unclear due to an obstruction, it may be necessary to perform a transesophageal echocardiogram. With TEE, the back of the throat is anesthetized and a scope is inserted. On the end of the scope is an ultrasonic device that a cardiologist will guide down to the lower part of the esophagus, where it is used to obtain a clearer, two-dimensional echocardiogram of the heart.
EECP (Enhanced External Counter Pulsation)
EECP is a therapy program that offers an alternative to surgery, particularly for patients who may not be good candidates for angioplasty or bypass surgery. EECP promotes circulation of blood to the heart to relieve coronary disease, angina and congestive heart failure as effectively as more common surgical procedures.
Patients receive EECP therapy while reclining on a bed with their legs and lower body wrapped in “cuffs” similar to those used for taking blood pressure readings. The cuffs are timed to inflate with air and deflate in coordination with the heart’s pumping rhythm. As the heart relaxes the cuffs inflate, circulating blood into the heart. When the heart pumps, the cuffs deflate, allowing the blood to flow freely through the legs and lower body. Treatments generally last one hour three to five times a week over a seven-week period.
Cardioversion

Pacemakers
A pacemaker is a small electrical device that is placed inside the body to help the heart maintain a regular beat. A pacemaker may be needed when you heart’s natural pacemaker is not working properly.
Your pacemaker will need to be checked periodically. Your cardiologist will provide all the information you will need for pacemaker care following implantation.
Defibrilators
A defibrilator is a permanent implant similar to a pacemaker, which can prevent life-threatening arrythmias, such as ventricular tachycardias, which can result in sudden death. Defibrilators are recommended for patients with weakened heart muscles and they re-establish the body’s natural pacemaker in the heart. For more information, or to see if you are a candidate for a defibrilator, consult with your cardiologist.
Treatments for Varicose & Spider Veins
Click to watch a Vascular Laser Therapy procedure to treat problem Varicose Veins
To see if laser vein therapy is right for you, call our office at 973-942-1141, send an email to veintreatment@hotmail.com and ask for more information, or submit a form from our Contact page.
Vein disease of the legs is one of the most common medical conditions. Approximately half of the population has some form of vein disease. Varicose veins affect up to 25% of all adults and about half of all people over 50. The most common cause of vein disease is heredity. Pregnancy, especially multiple pregnancies, is a contributing cause of vein disease. Other factors include age, obesity and jobs that require long periods of standing.
What causes vein disease?
Veins are the blood vessels that return blood to the heart from the Varicose veins body. To overcome the force of gravity, inside the veins are one-way valves which open to allow blood flow to the heart, and close to prevent “reflux” of blood back to the body. When these valves fail to function, or if the vein is damaged so the valves do not completely close, blood can begin to build up in the vein and cause a variety of vein complications, such as varicose veins and spider veins.
Varicose veins
Varicose veins are the large, “rope-like” veins that are often a quarter-inch in diameter. They can occur when veins do not properly return blood from the lower leg to the heart. When the valves inside the legs fail to work properly, blood leaks through and flows down the leg in the wrong direction, away from the heart. The blood overfills and distends the superficial veins under the skin, resulting in the bulging seen in varicose veins.
When varicose veins become severe, as in the photo shown here, the condition is referred to as chronic venous insufficiency. Symptoms of chronic venous insufficiency include aching pain, easy leg fatique and leg heaviness, all of which worsen as the day progresses.
Varicose veins generally continue to grow in size over time and can result in substantial pain and complications if not treated. Chronic venous insufficiency can cause ulcerations which can be very difficult to treat.
Spider veins
Spider veins are the small, thread-like colored veins that are most often seen on the surface of the skin. While many people seek treatment for spider veins for cosmetic reasons, spider veins also can result in substancial discomfort requiring therapy.
Treatments
Depending on the type and stage of vein disease, there are many different treatments. Here is a brief summary, which your physician can explain in more detail.
Compression Stockings
For minor pain from varicose veins, a compression stocking may be beneficial. The compression stocking will assist the leg in the pumping of blood back to the heart. While the vein disease symptoms may be relieved, compression stockings will not make the varicose veins go away.
Sclerotherapy
Sclerotherapy is used commonly for spider veins and smaller varicose veins. It involves injecting a small volume of liquid into the diseased vein. The sclerosing liquid acts upon the lining of the vein to cause it Spider Vein treatment, before and afterto seal shut, eliminating the vein completely. Sclerotherapy is quickly performed in a physician’s office and no anesthesia is required.
Because there are many veins in the leg, the blood that would have flowed through the closed vein simply flows through other healthy veins after the procedure. The loss of the diseased vein is not a problem for the circulatory system.
Laser Therapy to remove Varicose Veins
In the last few years, the use of lasers has become an accepted alternative to surgical stripping to treat varicose veins.
Vascular laser therapy can be performed in a physician’s office in less than one hour and the patient is encouraged to walk immediately following the procedure. In vascular laster therapy, a thin laser fiber is inserted into the diseased vein, generally through a small puncture in the leg above where the visual symptoms apear. The physician then delivers laser energy through the fiber, which causes the vein to close as the fiber is gradually removed.
Because there are many veins in the leg, the blood that would have flowed through the closed vein simply flows through other healthy veins after the procedure. The loss of the diseased vein is not a problem for the circulatory system.
Is vascular laser therapy painful?
Although individual responses vary, most people report feeling little or no pain after vascular laser therapy. Often the only sensation that is felt is during the deliveryof anesthetic to the leg. After the procedure, you may feel some tenderness, tingling, itching or tightness in the treated leg, which should disappear within a month.
How successful is vascular laser therapy?
Clinical results have been published which document the results of vascular laser treatment. Like any medical treatment, laser therapy has certain risks, which your doctor will explain to you as they may apply to your individual circumstances.
